Program Overview

The fellowship at NYP/Columbia offers one of the strongest abdominal organ transplant surgery training programs in the world. The program offers exceptionally strong training in liver, kidney, pancreas & hepatobiliary and robotic surgery. The clinical program covers the largest liver and kidney transplant programs in New York.
Dr. Jean C. Emond, Thomas S. Zimmer Professor of Surgery, Columbia University and The New York Presbyterian Hospital, is the Transplant Surgery Fellowship Program Director.
The fellowship program is among the most balanced training programs with fantastic opportunities in liver transplantation, living donor liver transplantation, kidney transplantation, living donor nephrectomy, hepatobiliary surgery, pediatric transplantation and pancreas transplantation. The training program is certified through the American Society of Transplant Surgeons (ASTS) in Liver/Kidney and HB surgery. We will provide financial support for any associated costs of licensing and credentialing. There are no senior residents or HPB fellows or Surgical oncology fellows on the service to diminish the training of the fellows.
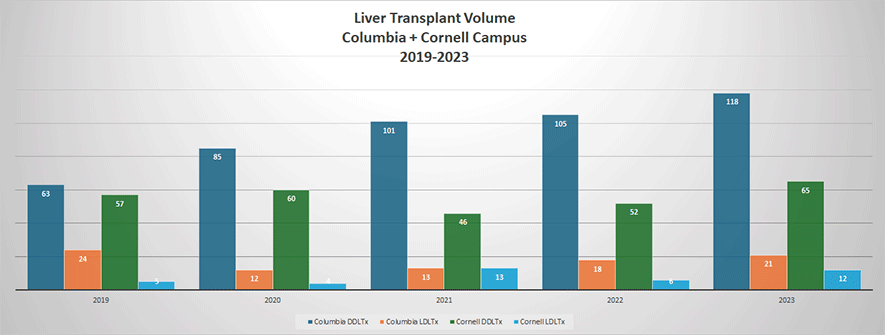
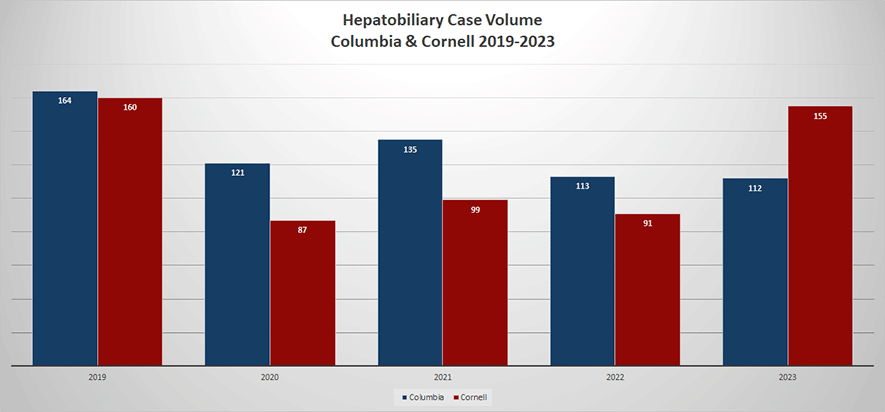
 The liver transplant program is one of the busiest programs in the country. With Dr. Jean Emond's leadership, the program has an international reputation for living donor liver transplant and hepatobiliary surgery. The Living Donor Liver Transplant Program is one of largest in the country and routinely performs robotic donor hepatectomies, under the leadership of Dr. Jason Hawksworth and Dr. Benjamin Samstein. The pediatric liver transplant program is one of the largest in the country and pediatric transplants are covered by the fellows. Approximately 150 hepatobiliary operations are performed each year by surgical staff. These include more than 75 hepatectomies. The program is certified as hepatobiliary training program through the ASTS.
The liver transplant program is one of the busiest programs in the country. With Dr. Jean Emond's leadership, the program has an international reputation for living donor liver transplant and hepatobiliary surgery. The Living Donor Liver Transplant Program is one of largest in the country and routinely performs robotic donor hepatectomies, under the leadership of Dr. Jason Hawksworth and Dr. Benjamin Samstein. The pediatric liver transplant program is one of the largest in the country and pediatric transplants are covered by the fellows. Approximately 150 hepatobiliary operations are performed each year by surgical staff. These include more than 75 hepatectomies. The program is certified as hepatobiliary training program through the ASTS.
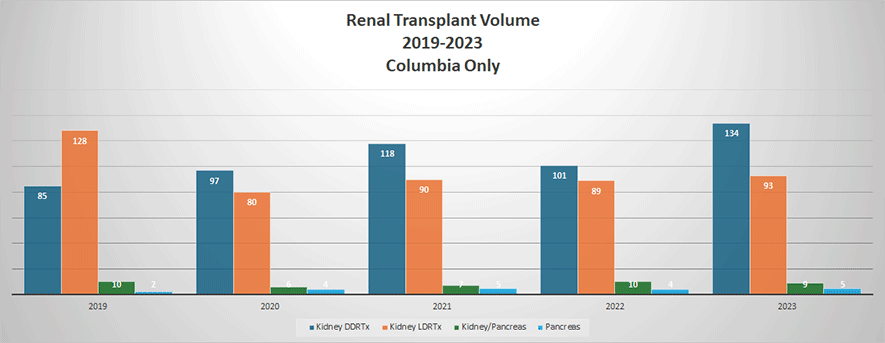
The kidney and pancreas arm of the program offers an equally broad experience. Under the guidance of Dr. Lloyd Ratner, Professor of Surgery, the Renal and Pancreas Transplant Program exposes the fellows to a wide range of kidney transplants. We perform approximately 125 live donor compatible transplants and approximately 125 deceased donor renal transplants. Dr. Ratner pioneered the use of laparoscopy for donor nephrectomy. All the living donor nephrectomies are performed by transplant staff and ASTS fellows. The pancreas program is substantial and performs 10-15 pancreas transplants annually.
 Fellows also gain experience in Intestinal Transplantation as well as Ex Vivo Oncological Service with Dr. Tomoaki Kato.
Fellows also gain experience in Intestinal Transplantation as well as Ex Vivo Oncological Service with Dr. Tomoaki Kato.
The services are well staffed with 24-7 PA coverage for all direct floor responsibilities. Fellows are responsible to supervise care along with PGY IV, III, II and I along with the Pas.
There are many opportunities for academic activities as well. The CCTI headed by Megan Sykes, MD was established in April 2010 and includes independent laboratories working in various areas of organ transplantation, hematopoietic cell transplantation, Type I diabetes, other areas of autoimmunity, tumor immunology and basic immunology. Clinical research in the areas of living donation, pediatric transplantation, antibody mediated rejection and tolerance with Dr. Josh Weiner is available as well.