Guide to Papillary Thyroid Cancer
Papillary thyroid cancer, which is the most common type of thyroid cancer, makes up about 80% of all cases of thyroid cancer. It is one of the fastest growing cancer types with over 20,000 new cases a year. In fact, it is the 8th most common cancer among women overall and the most common cancer in women younger than 25. Although a person can get papillary thyroid cancer at any age, most patients will present before the age of 40. Although risk factors for papillary thyroid cancer include radiation exposure and a family history of thyroid cancer, it is important to note that the majority of patients have no risk factors at all. Fortunately, papillary thyroid cancer is also the thyroid cancer with the best prognosis and most patients can be cured if treated appropriately and early enough. Up to 20% of patients will have involved lymph nodes at the time of diagnosis. However, unlike other cancers where involved lymph nodes means a very poor prognosis, in thyroid cancer involved lymph nodes usually have almost no impact on survival. Involved lymph nodes may increase the chance of recurrence (i.e. cancer coming back), but they do not change the prognosis. Most patients with papillary thyroid cancer will not die of this disease.
Signs and Symptoms
Most papillary thyroid cancers do not cause symptoms (i.e. they are asymptomatic). In fact, many patients will not know that they are there. Patients with large nodules may notice a palpable mass (i.e. a mass they can feel) or a visible mass (i.e. a mass they can see). Very large nodules may cause compressive symptoms which include difficulty swallowing, food or pills getting "stuck" when they swallow, and pressure or shortness of breath when lying flat. In cases of advanced cancer that are growing (i.e. invading) into surrounding structures, patients may develop hoarseness or difficulty swallowing. Enlarged neck lymph nodes that are concerning for cancer include those that are non-tender, firm, growing, and/or do not shrink over time. Patients with compressive symptoms, enlarged lymph nodes, hoarseness, and/or a rapidly growing nodule should seek medical evaluation right away.
Diagnosis
When a thyroid nodule is discovered, a complete history and physical examination should be performed. In particular, the doctor is looking for risk factors for cancer that include: a family history of thyroid cancer, a history of radiation exposure to the head, neck, and/or chest, age less than 20, age greater than 70, male gender, very hard nodules, enlarged lymph nodes, and/or hoarseness. After the history and physical exam, a TSH level should be checked to see if the patient is euthyroid (i.e. normal thyroid function), hyperthyroid (i.e. hyperactive or overactive thyroid), or hypothyroid (i.e. underactive thyroid). In general, it is unusual for hyperthyroid patients to have cancer while patients who are hypothyroid may have a slightly higher rate of cancer. Most patients with thyroid cancer are euthyroid.
The next step in the work-up of a thyroid cancer is an ultrasound (USG) of the neck. There is no radiation associated with an USG. An USG is the best test to look at the thyroid and will allow the doctor to see the size of the thyroid and specific features of the nodule(s) including: size, number of nodules, if there are calcifications (calcium deposits), echotexture (i.e. how bright or dark it looks on USG), borders, shape, and if it is solid or cystic (i.e. fluid-filled). In general, USG findings that are concerning for thyroid cancer include microcalcifications (i.e. microcalcifications), hypoechoic nodules, hypervascularity (i.e. more blood vessels than normal), irregular borders, and enlarged suspicious lymph nodes.
The best test to determine if a thyroid nodule is benign or cancer is a fine-needle aspiration biopsy (FNAB). In this test, a small needle (like the needles used for drawing blood) is placed into the nodule either by USG or feeling the nodule with the fingers. Cells are removed from the nodule into the needle (i.e. aspirated) and looked at under the microscope by a specially trained doctor called a cytologist. There are a number of different guidelines as to which nodules should be biopsied, but in general, nodules over 1 cm should be biopsied. If a patient has risk factors for thyroid cancer (especially a family history of thyroid cancer or exposure to radiation therapy) or suspicious findings on USG, then nodules over 0.5 cm should be biopsied. The FNAB may give one of 4 results:
-
Non-diagnostic:
This means that not enough cells were removed to make a diagnosis. Even in the best of hands, this happens in 5 to 10% of FNAB. Typically the FNAB will be repeated. If the nodule grows, then a repeat biopsy will usually be performed. In certain cases, a patient may go straight to an operation to make a diagnosis, especially if the risk of cancer is high or if the patient has had two or more non-diagnostic FNAB in the past.
-
Benign:
This means that there is a 97% chance that the nodule is not cancer. In most cases, patients with a benign biopsy are watched with an USG and physical exam 6 months later, and then at regularly scheduled times. A patient with a benign nodule may still have an operation if the nodule is large, causing symptoms, or cosmetically unappealing.
-
Malignant:
This means that there is a 97% chance that the nodule is cancer, usually a papillary thyroid cancer. Much less commonly, the FNAB can show a medullary or anaplastic thyroid cancer. Sometimes the cytologist reports that the nodule is "suspicious for thyroid cancer" which means that there is an 80 to 90% chance of cancer, again usually papillary thyroid cancer. Most patients with a FNAB of cancer will have a total thyroidectomy (i.e. removal of the entire thyroid) with or without removal of certain lymph nodes.
-
Indeterminate:
This category includes different readings like: follicular lesion, follicular neoplasm, Hurthle cell lesion, Hurthle cell neoplasm, and atypical cells or atypical lesions. This means that the cytologist cannot tell if the nodule is cancer, but the cells do not look normal. There is a 15 to 20% chance of having thyroid cancer with an indeterminate biopsy. Said another way, 1 out of 5 people with an indeterminate biopsy will have cancer. (See Follicular and Hurthle Cell Cancer »)
The only way to make a clear diagnosis of cancer or no cancer is to remove half or all of the thyroid and see if the cells in the nodule are invading (i.e. growing) outside of the nodule into the surrounding thyroid or outside of the thyroid. (See Thyroid Surgery »)
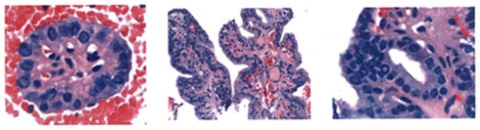
Microscopic views of normal thyroid tissue versus papillary thyroid cancer
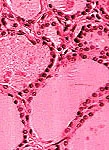
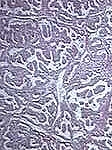
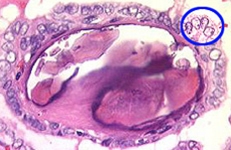
Of note, radioactive iodine (RAI) scans used to be performed routinely for patients with thyroid nodules because "hot" (i.e. hyperactive nodules) were rarely cancer (less than 1%) while "cold" (i.e. underactive nodules) carried a 10% risk of cancer. However, FNAB is far more accurate for determining the risk of cancer and RAI scans are mostly only used in cases of hyperthyroidism.
Treatment
There are three main parts to the treatment of papillary thyroid cancer:
Surgery:
The best treatment for papillary thyroid cancer is almost always total thyroidectomy (i.e. removal of the entire thyroid). There are a few very specific situations in which some doctors will remove only the half of the thyroid with the cancer (i.e. thyroid lobectomy), but most doctors recommend a total thyroidectomy because:
- Most papillary thyroid cancers are multifocal (i.e. in more than one part of the thyroid)
- Post-operative RAI ablation therapy is more effective if there is no normal thyroid tissue to soak up the radiation.
- Follow-up for recurrence (i.e. cancer that comes back) with the thyroglobulin blood test is more accurate. Thyroglobulin is a protein made by thyroid cells, both cancerous and normal. Without any normal thyroid tissue, the thyroglobulin level should be close to zero and if it rises, then it is likely that the cancer has come back. If there is half of a normal thyroid gland left in place, then the levels are harder to interpret and if the level rises, it will be unclear if the cancer has come back or if the normal thyroid lobe is growing.
- The recurrence rate (i.e. chance that cancer comes back) is lower in patients who have had a total thyroidectomy than a lobectomy.
In general, our preference at the Thyroid Center is to remove the entire thyroid gland in order to prevent the cancer from returning or spreading to the opposite side — but the extent of surgery is ultimately up to the patient. Prior to the operation, a lymph node mapping (i.e. an USG exam of the central and lateral compartments of the neck) should be done to see if there are suspicious lymph nodes that may need to be removed along with the thyroid. The most common location to have involved lymph nodes is in the central neck compartment (i.e. the lymph nodes surrounding the thyroid). If there are suspicious looking nodes on lymph node mapping or on inspection in the operating room, a therapeutic central neck dissection (i.e. removal of the central neck lymph nodes) should be performed. Some surgeons suggest removing all of the central neck lymph nodes regardless of whether or not they are suspicious looking in an operation called a prophylactic central neck dissection in order to lower the recurrence rate. However, most surgeons believe that a central neck dissection should only be done if there are suspicious looking lymph nodes because:
- The recurrence rate is essentially the same
- The complication rate is significantly higher in prophylactic central neck dissections versus therapeutic central neck dissections. See Thyroid Surgery > Risks of Thyroid Surgery
Risk of Complications With
Prophylactic vs Therapeutic Central Neck Dissection
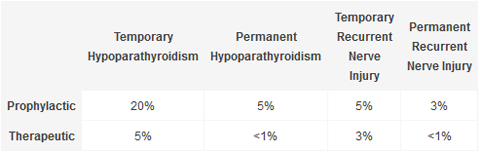

If the lateral neck lymph nodes (i.e. the lymph nodes surrounding the carotid artery and jugular vein) are involved with papillary thyroid cancer, then an operation called a modified radical neck dissection will be performed either at the time of the total thyroidectomy or in the future. This operation involves removing the lymph nodes along one side of the neck. After the operation, this area of the neck is usually numb for a period of time because the nerves to the skin in this area are purposely severed in order to remove the diseased lymph nodes. Other than this numbness, there are no long-term effects of having these lymph nodes removed.
Sometimes both the left and right lateral neck lymph nodes are involved with cancer. If this is the case, then modified radical neck dissections on one side and then the other are performed about 2 months apart. This delay is to allow time for healing on one side before operating on the opposite side. Performing the lymph node dissection on both sides at the same time could lead to unnecessary swelling (edema) of the head and face if time is not given between operations for alternate pathways of blood and lymph flow to form.
Thyroid Hormone Suppression:
After removal of the entire thyroid, patients will need to take thyroid hormone replacement pills (usually one pill a day for the rest of their lives) in order to replace the hormone that the thyroid would normally make. Patients with thyroid cancer are typically given a slightly higher dose than patients without thyroid cancer in order to suppress or block any stimulation for thyroid cancer cells to grow. The thyroid hormone replacement pill tricks the brain into thinking that enough thyroid hormone is being manufactured by the thyroid gland, therefore shutting down the brain's production of TSH (thyroid stimulating hormone which normally encourages the thyroid to make thyroid hormone). This is important because if TSH is left at high levels, it can stimulate both the remaining normal thyroid as well as any thyroid cancer and metastases to grow and enlarge. The thyroid hormone suppression dose for cancer is usually calculated to be 2 mcg/kg. In order to maintain a dose of thyroid hormone that is right for you, blood tests for thyroid function will need to be checked periodically. Generally, these blood tests are done every two months after surgery until a stable dose has been achieved, after which they may be done less frequently. Ask your doctor what is your correct individual dose.
Radioactive Iodine (RAI) Ablation:
Depending on the final pathology, the patient may need RAI ablation or what some doctors call remnant ablation. RAI ablation is not like the traditional external beam radiation which can be difficult on patients. RAI ablation is a pill that is taken once and usually causes few side effects. In this therapy, radioactive iodine is given to destroy any remaining thyroid cells (both cancer and benign) after total thyroidectomy. RAI ablation does not improve the overall excellent prognosis, but rather, it decreases the recurrence rate (i.e. chance of cancer coming back). Patients with papillary thyroid cancer larger than 4 cm in size, extrathyroid invasion (i.e. thyroid cancer that grows outside of the thyroid into surrounding tissue), thyroid cancer in lymph nodes (i.e. positive nodes), and/or thyroid cancer that has spread to other parts of the body (i.e. metastases) should have RAI ablation after total thyroidectomy. In general, papillary thyroid cancers less than 1 cm in size without positive nodes or extrathyroid invasion do not usually require RAI ablation. Patients with papillary thyroid cancers between 1 and 4 cm in size and/or that are multifocal should discuss with an experienced thyroid cancer specialist whether or not RAI ablation is needed. See RAI ablation ».
Fortunately, patients with papillary thyroid cancer rarely need chemotherapy or traditional external beam radiation therapy. External beam radiation is typically used in cases where the cancer has invaded into surrounding structures like the esophagus or windpipe (i.e. trachea). Finally, many people want to take an active role in their recovery from thyroid cancer. The Thyroid Center advises a healthy lifestyle and diet, including decreased alcohol consumption, avoiding cigarette smoking, and eating a diet which is low in fat and high in fiber. These changes are recommended to reduce many types of cancers, not just thyroid.
Follow-up
After surgery for papillary thyroid cancer, it is important to be examined regularly for signs that the cancer may have recurred. In general, patients should have a thyroglobulin blood test, TSH level, and USG of the neck every 6 months to a year. If the thyroglobulin level starts to go up, there are suspicious physical exam findings, or there are concerning nodules on USG, a RAI scan and/or FNAB may be done to determine if there is a recurrence.
Recurrence of Thyroid Cancer
Although thyroid cancer recurrence is not common, there are many treatment options available if it happens. If a cancer recurrence is detected in the neck lymph nodes, the best course of action is usually an operation to remove the affected node(s) or additional treatment with RAI ablation. In order to determine the best treatment for recurrent thyroid cancer, it is critical to work with an experienced team of thyroid specialists.
Next Steps
If you are dealing with a thyroid issue, our team at the Columbia Thyroid Center is here to help. Call (212) 305-0444 or request an appointment online.
Related Conditions
- Graves’ Disease
- Hyperthyroidism
- Hypothyroidism
- Multinodular Goiter
- Thyroiditis
- Thyroid Nodules
- Thyroid Cancer: Overview | Types | Causes | Symptoms | Diagnosis | Treatment | Prognosis/Outcomes
- Follicular Thyroid Cancer/ Hurthle Cell Carcinoma
- Medullary Thyroid Cancer
- Anaplastic Thyroid Cancer
- Thyroid Lymphoma
